 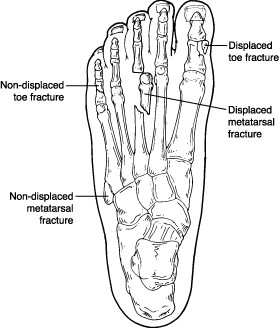 
While previous reports suggest that these injuries require a significant amount of force, recently, it has been suggested that there may be cases where the injury occurs more insidiously, possibly due to a stress-related phenomenon. Therefore, a high index of suspicion is key to recognizing and appropriately managing these injuries. These situations may result in failure to recognize the injury and ultimately a prolonged recovery due to inadequate treatment. Others may be more subtle injuries with insidious onset and lacking overwhelming clinical findings. Patients can present after an acute high-energy mechanism with significant swelling and ecchymosis. Turf toe injuries are now known to be caused by a variety of mechanisms. While it is still suggested that artificial turf results in a significant increase in risk of the injury, the recently reported incidence of turf toe injury is around 0.45–0.53 players per team each season. In the 1970s, the incidence was reported to be as high as 5–6 players per team each season with 30–45% of NFL players reporting a history of such injury and up to 83% of these injuries occurring on artificial turf. A recent retrospective review among NCAA football athletes suggested that the incidence has decreased in this population due to changes in shoe wear as well as improvements in artificial turf. The mechanism of injury was determined to be hyperdorsiflexion of the hallux combined with an axial load such as when a player falls back onto his own heel with his toe hyperextended and heel in equinus or steps out onto another players foot resulting in toe hyperextension (Fig. This was due to increasingly flexible shoes on a surface that did not give way like natural grass. Originally described in the 1970s, turf toe injuries were first recognized due to the use of artificial turf in the American football league. Injury to this complex can result in pain, weakness, and instability which can impact performance considerably. This force can increase up to 200–300% of the body weight with athletic activity and up to 800% with jumping. This small joint has been shown biomechanically to have joint reaction forces of up to 80% of the body weight through the toe-off phase of normal walking. The MTP joint provides balance during standing as well as essential power in the toe-off phase during activities from normal walking to jumping. These nerves lie on their respective side of the EHL tendon and have been shown in cadaver studies to be, on average, 3.4 and 4 mm from standard dorsolateral and dorsomedial metatarsophalangeal joint arthroscopy portal sites, respectively. 
The dorsomedial cutaneous nerve is an extension of the superficial peroneal nerve whereas the dorsolateral cutaneous nerve is an extension of the deep peroneal nerve. The medial and lateral proper digital nerves arise from the medial plantar nerve and run deep to the transverse metatarsal ligament. The fibrocartilaginous plantar plate allows for smooth gliding of the sesamoids and also provides stability through its connections with the deep transverse metatarsal ligament, the flexor tendon sheaths, and the plantar aponeurosis. This articulation also acts to off-load some of the forces through the MTP joint. The sesamoids are embedded within the FHB tendon slips and articulate with the plantar metatarsal head. The sesamoids act to increase the lever arm of the flexor hallucis brevis (FHB) and provide protection to the FHL tendon, which runs plantar between the sesamoids on the plantar aspect of the great toe. The sesamoids form through multiple ossification centers and are supplied by the sesamoid artery, which is a terminal branch of the medial plantar artery. The plantar plate capsuloligamentous complex contains the larger medial/tibial sesamoid and the smaller, rounder, and slightly more proximal lateral/fibular sesamoid. The extensor hallucis longus (EHL) and the flexor hallucis longus (FHL) cross the joint at the midpoint directly dorsal and plantar and insert on the distal phalanx. There are two tubercles on the plantar aspect of the proximal phalanx, adjacent to the articular surface, allowing muscular attachments (extensor and flexor hallucis brevis, intrinsics, and the adductor and abductor halluces). An intraarticular meniscus is commonly seen and is believed to enhance stability. Stability is provided mainly by the ligamentous and soft tissue structures spanning the joint with little stability provided by the shallow articulation. 
The proximal articular surface of the proximal phalanx has a concave shape that matches the transversely oriented metatarsal head, which is larger in the transverse plane than in the dorsoplantar plane. The hallux metatarsophalangeal (MTP) joint is a ginglymoarthrodial joint, meaning a ball and socket hinged joint with a sliding component. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
